You open your mailbox with dread. There’s the envelope with the hospital’s return address. It’s your bill, and it isn’t pretty.
Ever wonder how that bill was made?
Sure, there’s the cost of the procedure, doctor’s fees. Insurance plays a role. Then, there’s the envelope in your mailbox.
But what brings it all together? How is everything calculated?
Medical billing is more complicated than most people realize. But you’re in luck. This article will demystify six of the biggest billing mysteries.
Medical Billing is a Separate Industry
Doctors and nurses may make diagnoses, but they don’t make your bill. They do, however, keep records. Billers use these records to create an invoice, also called a claim.
This claim is then processed and sent to your insurance company. They will either accept or deny it. If they accept, the insurance company will pay out based on your policy.
Sounds simple, right?
Well, it isn’t. If the invoice has errors, insurance may deny the claim, forcing the doctor’s office to pass the entire bill to you. Scammers may also try to bill insurance for much more than the services rendered.
These issues have led to the growth of the medical billing industry. Doctors can shop different companies dedicated to making bills. They can even leave a medical billing service review.
It Has Its Own Codes
We mentioned earlier that clerks use medical records to make an invoice. But they don’t copy the doctor’s notes word for word. Instead, they use code.
Medical coding details everything: diseases, symptoms, diagnoses. Billers then use it in conjunction with hospital care procedures, each of which has a price.
The current code is the ICD-10, the International Classification of Diseases, 10th revision. It’s an updated version based on the WHO’s classification of diseases (the World Health Organization not the band).
The codes are structured using three to seven digits and letters. The numbers and letters correspond to over 68,000 diagnostic categories.
Why use a code?
It prevents disputes and provides an easy reference for billers, doctors, and insurance. A quick Google search can even help you learn these codes.
It Helps the Hospital
Hospitals aren’t a gold mine. You’d think they would be, right? Americans spend millions on healthcare.
But hospitals lose even more due to poor billing practices. In fact, most are more cash-strapped than they were during the financial crisis ten years ago.
Good billers keep hospitals and doctor’s offices afloat. They ensure compensation to these places for what they’re owed.
They help you, too.
Bills only charge for services rendered. It prevents you from paying any unnecessary medical costs.
It is All Digital
A long, long time ago–during the ’90s–billers made invoices using pen and paper. They had filing cabinets full of paperwork, insurance information. It was clutter heaven.
Nowadays, we do it differently.
Every bill is stored online, often using the latest software. Doctor’s use it, too.
It allows them to view insurance information, generate reports, even write a prescription. Billing software has fantastic security features, and most have access to the cloud, for use anywhere.
Billing Clerks are in Demand
Medical billing is a tedious process. Managing so many accounts and dealing with insurance is a full-time job.
Interested?
The Department of Labor expects a 9% growth rate by 2026. Moreover, it doesn’t take much to become a medical biller.
You need certification and an associate’s degree, at a minimum. Then, grab some experience. On average, medical billers make about $37,000 a year.
It’s not the highest salary in the world, but it’s steady work in a growing industry. You can’t beat that. Nor can you put a price on the value billers contribute to healthcare.
Medical Billing Determines What You Pay
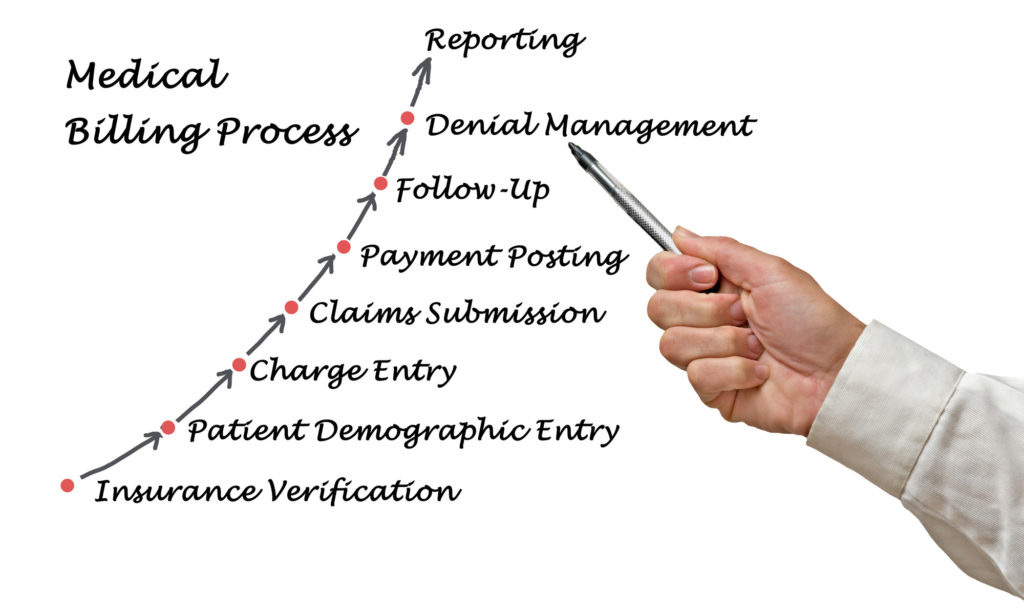
We’ve talked at length about billing, its ins and outs, how it affects the hospital. But how does it affect you?
It starts with the doctor’s visit. From here, you’ll register with the office’s system if you’re new. The system stores information on returning patients. They only need to describe the nature of their visit.
The next step is to establish financial responsibility. This part requires your insurance card. It’ll let the billers know where to send their claim and the nature of your policy.
They’ll also let you know if a co-pay is required. Afterward, you visit the doctor, then go home.
While you’re at home, billers create the invoice we mentioned earlier. They do an inventory on all services rendered. This inventory is called a superbill.
They then translate it to code, check it for compliance, and send it to your insurance company. Insurance will then accept or deny the claim.
You are responsible for whatever insurance doesn’t pay. Your bill will detail your obligations, the insurance payment, and a due date for your payment.
Final Thoughts
Medical billing seems complicated, but it isn’t. It’s just boring. Yet, it plays a vital role in the healthcare industry, making sure you pay for what you received.
The process is simple, the software’s simple to use, and the industry itself is on the rise. Who knew entire companies could base their business models on making bills?
Learning about the billing process will also give you more knowledge for your next check-up. Why stop there?
At Curiosity Human, our articles let you learn about everything. Wondering about computer upgrades? Need tips to battle exhaustion?
We’ve got it all and more. Check out our blog today. You’ll be smarter for it.